AFOs – When Splints Aren’t Just Splints
AFO = Ankle Foot Orthosis
Hearing the word ‘splint’ people often picture a rigid, single, simple brace. But rather, Ankle Foot Orthoses (AFOs) come in multiple shapes and forms – each with their own characteristics created to support specific clinical needs.
The correct AFO can significantly improve walking efficacy, comfort, stability and long-term joint health.
What is an AFO?
An AFO is a form of brace worn on the lower limb/s. When scripted properly an AFO can:
Improve gait pattern and quality
Support weak muscles
Control joint positioning
Prevent contractures
Reduce falls risk
Improve energy whilst mobilising
AFOs are commonly seen in multiple conditions across the lifespan. Some examples include stroke, multiple sclerosis (MS), cerebral palsy (CP) and foot drop.
Common AFOs:
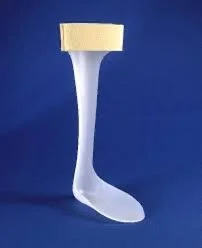
1. Flexible AFO
Designed to allow more natural movement
Providing mild support
Often used for mild foot drops, minor instability and clients who still have some active mediolateral muscular control preserved.
Some examples include; a posterior leaf spring (PLS) AFO, foot up splint and dictus band
These AFOs are often off the shelf and can be used as interim support whilst a customised splint is being created.
2. Rigid AFO
This type of AFO is custom made and allows no movement at the ankle
Rigid AFOs provide maximum control and stability but can feel restrictive. These are often prescribed and used when joint integrity and safety are the priority.
Common conditions include cerebral palsy, stroke, traumatic brain injury
GRAFO (ground reaction ankle foot orthosis) is a type of rigid AFO that has an anterior shell (part of the brace on the shin, rather than calf area) which spreads the load differently to a regular rigid AFO. The force is instead distributed to the front of the shin, which assists in extending the knee and maintaining ankle in a plantar grade position.
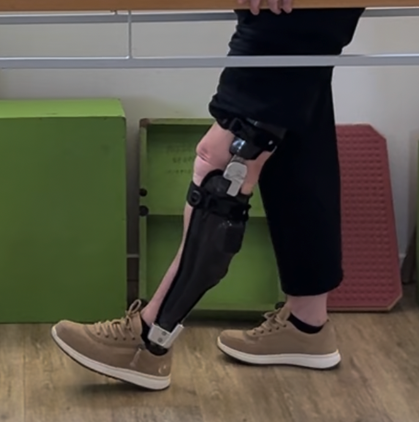
3. Hinged / Jointed AFO
This type of AFO includes an ankle joint hinge allowing some movement at the ankle (plantarflexion/dorsiflexion).
Best used for client who need support but will still benefit from ankle motion. It can improve gait mechanics and reduce knee hyperextension.
Commonly seen in conditions such as stroke, cerebral palsy, multiple sclerosis, traumatic brain injury, foot drop
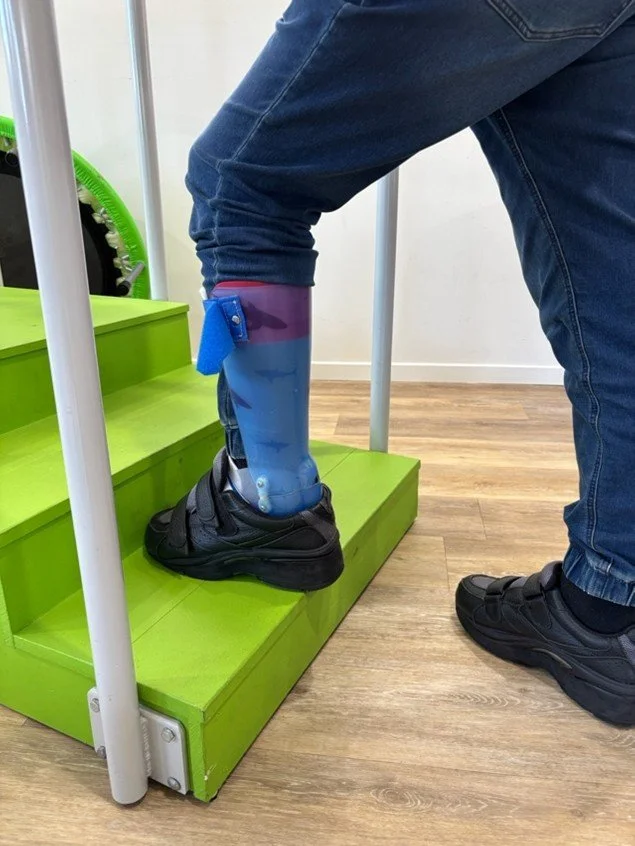
4. Dynamic AFO
These types of AFOs are often made from materials like carbon fibre which can be a lightweight, rigid yet flexible brace for longer distance walking
The orthosis assists with dorsiflexion, promoting a more natural gait and provides some stability.
Ideal option for active individuals with neurological conditions such as stroke
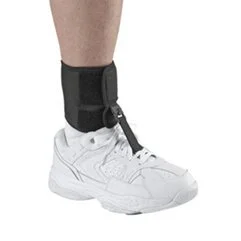
5. Step on AFO
Assists with active dorsiflexion (lifting toes/foot up).
These type of AFOs have a spring mechanism that assists in lifting the foot – which is customisable.
This has adjustable spring hinges
Often can be purchased off the shelf
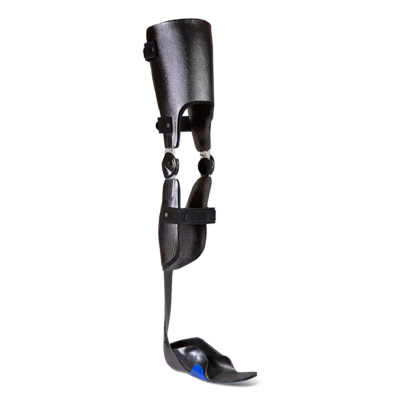
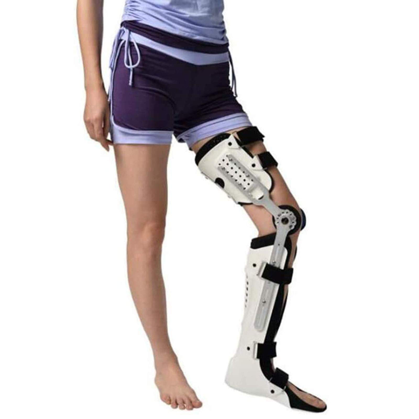
6. KAFO
Sometimes an ankle foot orthosis does not provide enough stability and effect – the KAFO (knee and ankle foot orthosis) provide support at both the knee and ankle.
These are sometimes used when there is excessive quad weakness, severe knee hyperextension and/or complex neurological presentations
A range of materials can be used – including metal, carbon fibre or plastic designs
These can be set to “lock” at the knee during weightbearing and is free moving whilst swinging. KAFOs can also utilise mechanics for assistance with gait
Assessments are completed with orthotists, often in conjunction with your therapists at Neuro Junction, to ensure the best option is provided.
There is no one-size-fits-all AFO
Physiotherapy and orthotic assessment considers the nature of condition (e.g. progressive, degenerative), muscle strength, balance, tone/spasticity, pain, range of movement, gait pattern, goals/lifestyle, footwear and skin integrity.
The Role of The Occupational Therapist
1. Assessment of function
OTs often assess how an AFO will help a person with:
Walking safety
Transfers
Balance
Participation in daily activities (e.g., dressing, bathing, community mobility)
2. Training and use
OTs commonly help patients:
Learn how to put on and remove the AFO
Integrate it into daily routines
Practice functional tasks like stairs, standing at a bench, or getting in/out of a car.
3. Equipment and footwear advice
OTs may advise on:
Footwear compatibility
Dressing aids or techniques
Environmental modifications if mobility is affected.